Understanding the disconnect between clinical activity and financial performance in healthcare
Introduction
Many healthcare organizations are experiencing a confusing pattern:
Patient volume is strong.
Schedules are full.
But cash flow is inconsistent.
This is one of the most searched, and least understood issues in medical practice financial performance and revenue cycle management. High volume does not guarantee strong cash flow. The reason lies in how revenue actually moves and leaks through the system.
The Disconnect Between Volume and Revenue
Healthcare revenue is not realized at the point of care. It flows through multiple stages:
- eligibility verification
- documentation and coding
- claim submission
- payer adjudication
- payment posting
- accounts receivable follow-up
Each step introduces time delay + risk of revenue loss.
Key Metric: Days in A/R (DSO)
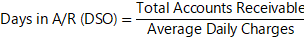
What this means:
- Ideal: 30–40 days
- Concerning: >50 days
- High risk: >70 days
The higher your DSO, the more unpredictable your cash flow becomes.
Why Cash Flow Becomes Unpredictable
1. Payer Delays and Variability
Even clean claims are not paid consistently.
Example:
- Medicare: ~14–21 days
- Commercial payers: 30–60+ days
- Denied/reworked claims: 60–120 days
Same work → different timelines → unstable cash flow
2. Accounts Receivable Inefficiencies
A/R is where cash flow is either stabilized or lost. Even a 10% inefficiency in A/R follow-up creates significant financial impact.
Example: Revenue Loss from A/R Gaps
Let’s take a $5M annual practice:
- Monthly revenue: ~$416,000
- If 10% of claims are delayed or not followed up properly:
> Monthly impact: ~$41,600
> Annual impact: ~$ 416,000
This is not lost production. This is revenue already earned but not collected.
3. Denial Management Gaps
Industry denial rates:
- Average: 5–10%
- Poorly managed systems: >12–15%
But more important is recovery rate. If:
- 10% of claims denied
- Only 60% recovered
4% of total revenue is lost permanently
Example: Denial Impact
For a $5M practice:
- 10% denied = $500,000
- 40% unrecovered = $200,000 loss
Direct impact on cash flow and profitability.
4. Front-End Errors (Biggest Hidden Driver)
Revenue leakage often starts before the visit:
- eligibility not verified
- authorization missing
- incorrect patient data
These errors lead to:
- delayed claims
- denials
- rework cycles
increasing time to payment.
Critical Performance Metrics to Track
High-performing organizations monitor:
- Net Collection Rate
- Target: >95%
- First Pass Resolution Rate
- Target: >90%
- Denial Rate
- Target: <5%
- % A/R > 90 Days
- Target: <15–20%
The Visibility Problem
Most organizations track:
- charges
- collections
- A/R
But they lack clarity on:
> where revenue is delayed
> how much is at risk
> which workflow is responsible
The Real Financial Equation
Cash flow is not based on production. It is based on:
Cash Flow = Collected Revenue ÷ Time + Efficiency of Revenue Cycle
The Strategic Shift
High-performing organizations treat revenue as a system, not a task.
They focus on:
- workflow alignment
- A/R discipline
- denial recovery systems
- real-time financial visibility
- accountability across teams
Final Thought
Unpredictable cash flow is not a volume problem. It is a revenue system problem.
Pract-Eaze Perspective
Pract-Eaze works with private practices, healthcare organizations, and EMR partners to improve cash flow predictability, revenue visibility, and financial performance.
📞 724-512-5777
✉️ info@pract-eaze.com
🌐 www.pract-eaze.com
Closing Line
The revenue is already being generated.
The question is: how much of it are you actually collecting?
Dr. Renu Joshi, MD, EMBA, FACOG
OB-GYN | Private Practice Physician | Physician-Entrepreneur
Founder, Pract-Eaze
Recent Posts
The most recent content on our blog, showcasing a variety of articles, insights, and resources to inform and inspire our readers.
-

Upcoming Virtual Talk: New AMA Coding Guidelines, Jun 6 2026
The landscape of Obstetric billing may be entering one of its most significant transitions in…
-

AMA Obstetric Coding Changes 2027: Revenue Impact Across Practices, Health Systems, and EMR Platforms
A strategic analysis of how the shift from global OB packages to encounter-based coding will…
-

Upcoming Talk: Coding Demystified, May 12 2026
Office Coding Demystified: Mastering Annual Exams and E/M Visits Accurate medical billing and coding are…
